InVivoMAb anti-mouse CD1d (CD1.1)
Product Details
The 20H2 monoclonal antibody reacts with mouse CD1d also known as CD1.1. CD1d is a 48 kDa type I membrane glycoprotein and a member of the CD1 family of glycoproteins. CD1d is a non-classical MHC protein with structural homology to class I MHC molecules. CD1d is expressed on the surface of various antigen-presenting cells and is involved in the presentation of non-peptide glycolipid antigens to to CD1d-restricted T cells. CD1d-presented glycolipid antigens activate invariant natural killer T (iNKT) cells, through the interaction with the T-cell receptor present on iNKT cell membranes. When activated, iNKT cells rapidly produce Th1 and Th2 cytokines.Specifications
| Isotype | Rat IgG1, κ |
|---|---|
| Recommended Isotype Control(s) | InVivoMAb rat IgG1 isotype control, anti-horseradish peroxidase |
| Recommended Dilution Buffer | InVivoPure pH 7.0 Dilution Buffer |
| Conjugation | This product is unconjugated. Conjugation is available via our Antibody Conjugation Services. |
| Immunogen | CD1.1-transfected rat cell line RBL-CD1.1 followed by CD1.1-transfected human cell line CR1-CD1.1 |
| Reported Applications |
iNKT cell neutralization in vivo CD1d blockade Flow cytometry |
| Formulation |
PBS, pH 7.0 Contains no stabilizers or preservatives |
| Endotoxin |
<2EU/mg (<0.002EU/μg) Determined by LAL gel clotting assay |
| Purity |
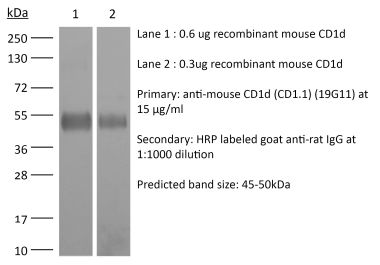
>95% Determined by SDS-PAGE |
| Sterility | 0.2 µm filtration |
| Production | Purified from cell culture supernatant in an animal-free facility |
| Purification | Protein G |
| RRID | AB_10949293 |
| Molecular Weight | 150 kDa |
| Storage | The antibody solution should be stored at the stock concentration at 4°C. Do not freeze. |
Recommended Products
iNKT cell neutralization
Pilones, K. A., et al. (2014). "Invariant natural killer T cells regulate anti-tumor immunity by controlling the population of dendritic cells in tumor and draining lymph nodes" J Immunother Cancer 2(1): 37. PubMed
BACKGROUND: Invariant natural killer T (iNKT) cells are CD1d-restricted T cells, which respond rapidly to antigen recognition and promote development of anti-tumor immunity in many tumor models. Surprisingly, we previously found that mice deficient in iNKT cells developed spontaneous CD8(+) T cells responses partially effective at inhibiting metastases in mice bearing the 4T1 mammary carcinoma, and showed a markedly improved response to treatment with local radiotherapy and anti-CTLA-4 antibody compared to wild type (WT) mice. METHODS: To understand the mechanisms of the immunosuppressive function of iNKT cells, dendritic cells (DCs) were analyzed by immunohistochemistry and flow cytometry in WT and iNKT-deficient (iNKT(-/-)) mice. The effects of antibody-mediated blockade of CD1d on DC number and phenotype, priming of anti-tumor T cells, and tumor response to treatment with local radiotherapy and anti-CTLA-4 antibody were evaluated. To determine if the improved response to treatment in the absence of iNKT cells was independent from the immunotherapy employed, 4T1-tumor bearing WT and iNKT(-/-) mice were treated with local radiotherapy in combination with antibody-mediated CD137 co-stimulation. RESULTS: DCs in 4T1 tumors and tumor-draining lymph nodes but not distant lymph nodes were significantly reduced in WT mice compared to iNKT(-/-) mice (p < 0.05), suggesting the selective elimination of DCs cross-presenting tumor-associated antigens by iNKT cells. Consistently, priming of T cells to a tumor-specific CD8 T cell epitope in mice treated with radiotherapy and anti-CTLA-4 or anti-CD137 was markedly enhanced in iNKT(-/-) compared to WT mice. CD1d blockade restored the number of DC in WT mice, improved T cell priming in draining lymph nodes and significantly enhanced response to treatment. CONCLUSIONS: Here we describe a novel mechanism of tumor immune escape mediated by iNKT cells that limit priming of anti-tumor T cells by controlling DC in tumors and draining lymph nodes. These results have important implications for the design of immunotherapies targeting iNKT cells.
iNKT cell neutralization
Hayworth, J. L., et al. (2012). "CD1d-independent activation of mouse and human iNKT cells by bacterial superantigens" Immunol Cell Biol 90(7): 699-709. PubMed
Invariant NKT (iNKT) cells are infrequent but important immunomodulatory lymphocytes that exhibit CD1d-restricted reactivity with glycolipid Ags. iNKT cells express a unique T-cell receptor (TCR) composed of an invariant alpha-chain, paired with a limited range of beta-chains. Superantigens (SAgs) are microbial toxins defined by their ability to activate conventional T cells in a TCR beta-chain variable domain (Vbeta)-specific manner. However, whether iNKT cells are directly activated by bacterial SAgs remains an open question. Herein, we explored the responsiveness of mouse and human iNKT cells to a panel of staphylococcal and streptococcal SAgs and examined the contribution of major histocompatibility complex (MHC) class II and CD1d to these responses. Bacterial SAgs that target mouse Vbeta8, such as staphylococcal enterotoxin B (SEB), were able to activate mouse hybridoma and primary hepatic iNKT cells in the presence of mouse APCs expressing human leukocyte antigen (HLA)-DR4. iNKT cell-mediated cytokine secretion in SEB-challenged HLA-DR4-transgenic mice was CD1d-independent and accompanied by a high interferon-gamma:interleukin-4 ratio consistent with an in vivo Th1 bias. Furthermore, iNKT cells from SEB-injected HLA-DR4-transgenic mice, and iNKT cells from SEB-treated human PBMCs, showed early activation by intracellular cytokine staining and CD69 expression. Unlike iNKT cell stimulation by alpha-galactosylceramide, stimulation by SEB did not induce TCR downregulation of either mouse or human iNKT cells. We conclude that Vbeta8-targeting bacterial SAgs can activate iNKT cells by utilizing a novel pathway that requires MHC class II interactions, but not CD1d. Therefore, iNKT cells fulfill important effector functions in response to bacterial SAgs and may provide attractive targets in the management of SAg-induced illnesses.
iNKT cell neutralization, Flow Cytometry
Yang, W., et al. (2011). "NKT cell exacerbation of liver metastases arising from melanomas transplanted into either the eyes or spleens of mice" Invest Ophthalmol Vis Sci 52(6): 3094-3102. PubMed
PURPOSE: To explore the role of natural killer T (NKT) cells in the development of liver metastases in mice harboring intraocular melanomas. METHODS: Cells derived from the cutaneous B16 melanoma cell line (B16LS9) were transplanted either into the vitreous body or under the spleen capsules of wild-type C57BL/6 mice and NKT-cell-deficient Jalpha18(-/-) and CD1d(-/-) mice. The development of liver metastases was evaluated by histopathology. The effect of NK cells on liver metastases was determined by selective depletion with anti-asialo-GM1 antiserum in vivo and NK-cell-mediated cytolysis of B16LS9 melanoma cells in vitro. The role of IL-10 and transforming growth factor (TGF)-beta in the inhibition of liver NK resistance to liver metastases was determined by in vivo and in vitro neutralization with monoclonal antibodies. RESULTS: Liver NKT cells, especially type I NKT cells, enhanced liver metastases arising from intraocular melanomas. NKT-cell-deficient mice developed significantly fewer liver metastases that were NK-cell dependent. Tumor-induced liver NKT cells, especially type I NKT cells, inhibited liver NK-cell cytotoxicity by an IL-10-dependent process. CONCLUSIONS: NKT cells exert protective effects in many murine tumor models. However, the present results reveal that NKT cells exacerbate liver metastases arising from intraocular melanomas. To the authors’ knowledge, this is the first report that liver NKT cells, especially type I NKT cells, inhibit liver NK-cell antimetastatic activity by the production of IL-10. These results suggest that hepatic NKT cell activity can have an important effect in the immune surveillance of liver metastases.
iNKT cell neutralization, Flow Cytometry
Miellot-Gafsou, A., et al. (2010). "Early activation of invariant natural killer T cells in a rheumatoid arthritis model and application to disease treatment" Immunology 130(2): 296-306. PubMed
Invariant NKT (iNKT) cells are a distinctive subtype of CD1d-restricted T cells involved in regulating autoimmunity and capable of producing various T helper type 1 (Th1), Th2 and Th17 cytokines. Activation of iNKT cells by their exogenous ligand alpha-galactosylceramide (alpha-GalCer) exerts therapeutic effects in autoimmune diseases such as rheumatoid arthritis (RA). However, the pathophysiological role of iNKT cells in RA, in the absence of exogenous stimulation, is incompletely understood. We investigated the potential pathophysiological effects of iNKT cells in mice with collagen-induced arthritis (CIA), a model of RA. We found that iNKT cells underwent activation only in the early phases of the disease (6 days post-induction). In the liver, but not the spleen or lymph nodes, this early activation led to the release of interleukins -4, -17A and -10 and of interferon-gamma; and an increased CD69 expression. Importantly, clinical and histological signs of arthritis were improved by the functional blockade of iNKT cells by a monoclonal antibody to CD1d at the early phase of the disease. This improvement was associated on day 6 post-induction with decreased expression of co-stimulatory molecules (CD80, CD86, CD40) on splenic dendritic cells and macrophages, whereas regulatory T-cell suppressive effects and proportions were not modified. Taken in concert, these findings suggest that iNKT cells are activated early in the course of CIA and contribute to the pathogenesis of arthritis. Therefore, iNKT-cell activation may be a valid treatment target in RA.
in vivo CD1d blockade
Shi, M. Q., et al. (2006). "Experimental African trypanosomiasis: lack of effective CD1d-restricted antigen presentation" Parasite Immunol 28(12): 643-647. PubMed
BALB/c mice are highly susceptible to African trypanosomiasis, whereas C57BL/6 mice are relatively resistant. Other investigators have reported that the synthesis of IgG antibodies to purified membrane form of variant surface glycoprotein (mfVSG) of Trypanosoma brucei is CD1 restricted. In this study, we examine the role of the CD1d/NKT cell pathway in susceptibility and resistance of mice to infection by African trypanosomes. Administration of anti-CD1d antibodies to Trypanosoma congolense-infected BALB/c mice neither affects the parasitemia nor the survival time. Correspondingly, CD1d(-/-) and CD1d(+/+) BALB/c mice infected with T. congolense or T. brucei show no differences in either parasitaemia or survival time. The course of disease in relative resistant C57BL/6 mice infected with T. congolense is also not affected by the absence of CD1d. Parasitaemia, survival time, and plasma levels of IgG2a and IgG3 parasite-specific antibodies in infected CD1d(-/-) C57BL/6 are not different from those of infected CD1d(+/+) C57BL/6 mice. We conclude that CD1d-restricted immune responses do not play an important role in susceptibility/resistance of mice infected with virulent African trypanosomes. We speculate that virulent trypanosomes have an evasion mechanism that prevents the induction of a parasite-specific, CD1d-restricted immune response by the host.
in vivo CD1d blockade
D’Souza, C. D., et al. (2000). "A novel nonclassic beta2-microglobulin-restricted mechanism influencing early lymphocyte accumulation and subsequent resistance to tuberculosis in the lung" Am J Respir Cell Mol Biol 23(2): 188-193. PubMed
In this study, we compared the course of a low-dose aerosol Mycobacterium tuberculosis infection in mice bearing gene disruptions for the beta2-microglobulin molecule, the CD8 molecule, and the CD1 molecule. Over the first 50 d of infection, the CD8- and CD1-disrupted mice were no more susceptible to infection than were the control mice. In contrast, the bacterial load in beta2-microglobulin gene-disrupted mice increased rapidly and attained much higher levels than that observed in the other gene-disrupted mice and in control mice. A second major difference between the beta2-microglobulin gene-disrupted mice and the other animals was the development of lung granulomas; both the CD8- and CD1-disrupted mice developed essentially normal granulomas except for an apparent increased lymphocyte influx in the CD8-disrupted mice. The beta2-microglobulin gene-disrupted mice, on the other hand, developed granulomas virtually devoid of lymphocytes, with these cells instead localized within prominent perivascular cuffing adjacent to the lesions. These data support the hypothesis that a beta2-microglobulin-dependent, non-CD8- and non-CD1-dependent mechanism controls the early and efficient influx of protective lymphocytes into infected lesions, and that the absence of this mechanism decreases the capacity of the animal to initially deal with pulmonary tuberculosis.
in vivo CD1d blockade, Flow Cytometry
Szalay, G., et al. (1999). "Cutting edge: anti-CD1 monoclonal antibody treatment reverses the production patterns of TGF-beta 2 and Th1 cytokines and ameliorates listeriosis in mice" J Immunol 162(12): 6955-6958. PubMed
Protection against intracellular bacteria by T cells is regulated by Ag-presenting molecules, which comprise classical MHC class I molecules, MHC class II molecules, and nonclassical MHC class Ib molecules. The role of CD1 molecules, which are structurally similar to classical MHC class I gene products, but less polymorphic, is not understood so far. We show that CD1 surface expression increased on APC in Listeria-infected mice. The in vivo treatment with anti-CD1 mAb reduced TGF-beta 2 levels and concomitantly increased secretion of the proinflammatory cytokine TNF, the Th1 cell promoting cytokine IL-12, and the Th1 cell cytokine IFN-gamma at the onset of listerial infection. These findings point to a regulatory role of CD1-reactive cells in the immune response against listeriosis.